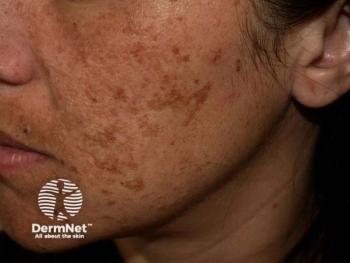
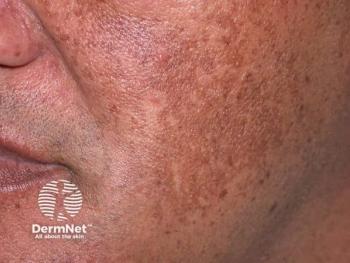
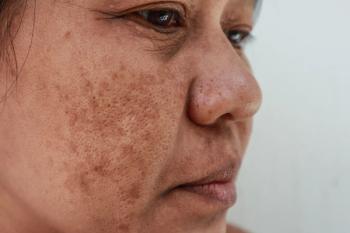
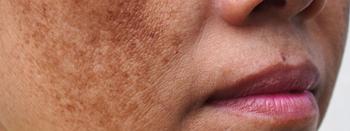
Facial pigmentation impacts quality of life regardless of clinical severity
In a study of more than 200 men and women, clinicians scored patients’ pigmentation taking into account how much of the face was impacted and compared scores to patients’ responses to the Skindex-16 questionnaire.
Facial pigmentary disorders, including melasma, impact quality of life for both men and women, but women tend to be emotionally more affected than men, according to a study published March-April in the Indian Dermatology Online Journal.
“As face is the most visible part of the body, any blemish on it can have a serious impact on the psychological wellbeing of the individual. Causes of facial melanosis are many and varied and each of them can have an impact on the quality of life,” said the study’s lead author Leena Raveendra, M.D., associate professor of dermatology at Rajarajeswari Medical College and Hospital, in Bangalore, Karnataka, India.
Dr. Raveenra and colleagues studied 186 women and 52 men diagnosed at the hospital in India with facial pigmentation from April 2015 to March 2016. While 73% of those studied had melasma, the most common of the pigmentary disorders, 5.8% of patients had post-inflammatory hyperpigmentation or photo tanning. Other diagnoses included lichen planus pigmentosus, freckles and Nevus of Ota. Researchers noted 0.42% of cases were diagnosed as acanthosis nigricans, Becker’s nevus, pigmentary demarcation lines, Nevus spilus, seborrheic melanosis, or post-chikungunya pigmentation.
RELATED:
The clinicians scored patients’ pigmentation taking into account how much of the face was impacted, pigmentary severity compared to normal skin, and pigmentation uniformity, including whether it was speckled or diffuse. Patients also responded to the Skindex-16 questionnaire, a proven instrument that measures quality of life in people with skin diseases.
Looking at patients’ quality of life, which can give dermatologists a perspective on patients’ feelings of joy and satisfaction, has become increasingly important in the management of patients with skin diseases, according to the paper. That’s especially true when it comes to facial skin disorders. The authors noted that other studies suggest people with facial skin conditions are at risk for depression, as well as feelings of loneliness and isolation.
“Melasma has been the focus of the studies on hyperpigmentation of the face. It is known to reduce the quality of life of the patients. Other causes of pigmentation have a similar or sometimes more impact on the quality of life,” Dr. Raveendra said.
Dr. Raveendra and colleagues found the quality of life impact happened regardless of pigmentation severity or how they scored facial pigmentation.
The mean pigmentation score was 20.39, with clinicians noting mild pigmentation in 41.17% of patients, compared to moderate in 42% and severe pigmentation in 16.8% of cases.
Patients’ mean Skindex score was 1.12, with a mean emotion score of 17.32. While the authors only noted a slightly higher mean Skindex-16 score among females in the study, they reported a more significant difference in emotion, with females scoring the emotional impact of pigmentary disorders higher than males. Mean skin index scores were highest for post-chikungunya pigmentation and lowest for melasma and post-inflammatory pigmentation.
There was only a weak positive correlation between the clinicians’ pigmentation score and Skindex-16.
“Skindex-16 score against different grades of pigmentation showed that the mean Skindex-16 score was higher in severe cases but there was no statistically significant difference between the groups,” they wrote.
Dr. Raveendra told Dermatology Times that the extent and severity of facial pigmentation in the study was not proportional to the severity of impairment of quality of life.
“Even a small blemish on the face can decrease the quality of life and have an impact on their psychological wellbeing,” she said.
Disclosure:
Dr. Raveendra reports no relevant disclosures.
Reference:
Raveendra L, Sidappa H, Shree S.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.