Erythrodermic Psoriasis: A Rare Disease
Erythrodermic psoriasis, affecting about 1-2% of psoriatic patients, is a rare, potentially life-threatening variant of psoriasis.
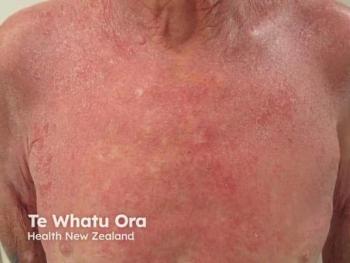
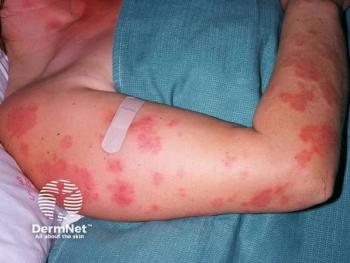
Erythrodermic psoriasis (EP), affecting about 1-2% of psoriatic patients, is a rare, potentially life-threatening variant of psoriasis. The condition is characterized by generalized redness and severe skin peeling, involving nearly 75-90% of the total body surface area.1 A study conducted in 2018 reported a higher prevalence of EP in Asians.2
Clinical Presentation:
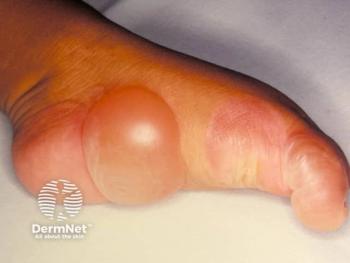
Patients with EP may present with generalized cutaneous symptoms, including erythema, scaling, pruritis, edema, psoriatic plaques, and exudative lesions.3 Nail dystrophies, particularly involving fingernails, are also common among these patients.4 Due to considerable cutaneous involvement, patients may present with systemic symptoms, such as fever, fatigue, lymphadenopathy, tachycardia, and arthralgia.1 Patients with EP are more likely to exhibit complications due to transepidermal fluid and nutrient loss, leading to multi-organ failure or even death in severe cases.5
Causes:
Although psoriasis is the most frequent cause of EP,6 several other triggering factors for developing EP have been identified, including infections, prolonged sun exposure, overuse or abrupt withdrawal of corticosteroids, drug reactions, and severe stress. However, a more recent study reported worsening of the condition following vaccination against COVID-19.7
Due to the paucity of data and the rarity of the disease, the exact pathogenesis of EP is yet to be understood. However, research revealed that increase in several biomarkers, including IL-4, IL-10, and serum IgE, may attribute a th1/th2 imbalance toward th2 differentiation and play a key role in the pathogenesis of the disease.4 Regarding the cause of the condition, Bernard Cohen, MD, Professor of Pediatrics and Dermatology at the Johns Hopkins University School of Medicine, said, “The cause is not always clear, but viral and bacterial infections, as well as certain medications, may trigger this explosion of psoriasis.”
Management:
EP is a medical emergency and requires immediate medical attention. While emphasizing the importance of immediate treatment, Cohen says, “Treatment is important to reduce the risk of serious systemic complications. Patients require systemic therapy and may respond well to traditional therapies, such as methotrexate (mtx), mycophenolate mofetil, and cyclosporine. Of these options, mtx is probably the safest and most effective.”
The initial steps in the treatment of EP include managing any protein or electrolyte imbalances, preventing hypothermia, and identifying and treating any secondary infections.5 Treatment options may include:
Biologics: Biologic therapies have shown promise in the treatment of EP. Biologics, including TNF-α inhibitors, IL-17, and IL-12/IL-23 blockers, have several benefits in treating EP over conventional therapies. Some benefits include rapid onset and long duration of action, high efficacy, few drug interactions, lesser associated toxicities and lesser frequency of administration.8 Cohen says, “The biologics provide good, relatively rapid responses, and if carefully selected, can be relatively safe. A number of these agents are being studied and approved for children too.”
Drug Therapy: Infliximab and cyclosporine are standard first-line therapies in managing EP; however, methotrexate and acitretin were considered in chronic cases to control cell growth. Although these agents are highly efficacious in disease management, possible associated complications and the advent of new targeted biologic therapies, especially IL-17 and IL-23 blockers, have limited their role. 8
Though there is limited data on the comparison of biologics and conventional treatment for managing EP, the choice of therapy is largely dependent on a range of factors, including patients’ age, affordability and availability of drugs.
Topical treatments: Together with systemic treatment, topical agents of moderate to high efficacy, such as steroids, vitamin D analogs, and emollients, may be beneficial in treating EP.
Phototherapy: Phototherapy is not recommended for acute cases and may increase the risk of koebnerization due to photosensitization. However, it can be considered a treatment option for long-term, stable cases. 9
References
- Lo Y, Tsai TF. Updates on the treatment of erythrodermic psoriasis. Psoriasis (Auckl). 2021;11:59-73. Published 2021 Jun 9. doi:10.2147/PTT.S288345
- Yan D, Afifi L, Jeon C, Cordoro KM, Liao W. A cross-sectional study of the distribution of psoriasis subtypes in different ethno-racial groups. Dermatol Online J. 2018;24(7):13030/qt5z21q4k2. Published 2018 Jul 15.
- Okubo Y, Umezawa Y, Sakurai S, Hoshii N, Nakagawa H. Efficacy and safety of certolizumab pegol in Japanese patients with generalized pustular psoriasis and erythrodermic psoriasis: 52-Week Results. Dermatol Ther (Heidelb). 2022;12(6):1397-1415. doi:10.1007/s13555-022-00741-x
- Tso S, Satchwell F, Moiz H, et al. Erythroderma (exfoliative dermatitis). Part 1: underlying causes, clinical presentation and pathogenesis. Clin Exp Dermatol. 2021;46(6):1001-1010. doi:10.1111/ced.14625
- Reynolds KA, Pithadia DJ, Lee EB, Liao W, Wu JJ. A systematic review of treatment strategies for erythrodermic psoriasis. Journal of Dermatological Treatment. 2019;32(1):49-55. doi:10.1080/09546634.2019.1689228
- Foss MG, Nyckowski T, Steffes W. Erythrodermic Psoriasis Exacerbated by Bupropion. Cureus. 2021;13(10):e18460. Published 2021 Oct 3. doi:10.7759/cureus.18460
- Tran TB, Pham NTU, Phan HN, Nguyen HT. Generalized erythrodermic psoriasis triggered by vaccination against severe acute respiratory syndrome Coronavirus 2. Dermatol Ther. 2022;35(6):e15464. doi:10.1111/dth.15464
- Dogra S, Mehta H. Biological treatment for erythrodermic psoriasis. Expert Opinion on Biological Therapy. 2022:1-13. doi:10.1080/14712598.2022.2128669
- Voloshyna D, Ehsan Ullah S, Jahan N, et al. Beta-Blocker-Induced Erythrodermic Psoriasis: A Case Report. Cureus. 2022;14(10):e29809. Published 2022 Oct 1. doi:10.7759/cureus.29809
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.