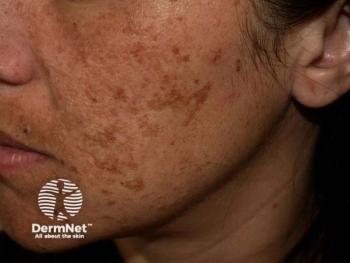
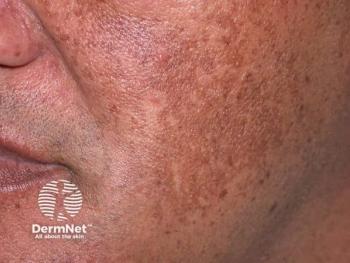
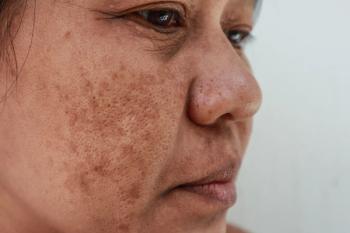
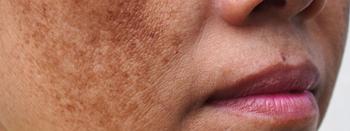
Diagnosing, managing hypopigmented skin disorders
Early diagnosis and appropriate management of hypopigmented skin disorders can improve a patient’s quality of life, halt disease progression and prevent irreversible disability.
Acquired hypopigmented skin changes are common, but recognizing underlying causes swiftly can benefit overall patient health. In some cases, it can be critical.
In
“Early diagnosis and appropriate management of these disorders can improve a patient’s quality of life, halt disease progression and prevent irreversible disability,” the author’s wrote.
Even in benign cases, these disorders can have significant cosmetic, psychological, economic, and societal impacts. Studies and biopsies often do not render a diagnosis, so dermatologists must rely on characteristic clinical features to determine the underlying cause.
INFECTIOUS CONDITIONS
Prompt treatment can alleviate these conditions.
Hypochromic pityriasis versicolor: This superficial fungal infection, caused by Malassezia spp., typically appears during or post-puberty and presents with hypopigmented macules on the neck, upper trunk, and extremities. Immunocompromised individuals can see macules on the lower extremities and face. Risk factors include hyperhidrosis, endocrinopathies, oral contraceptives, depressed cellular immunity and oily preparation applications.
Topical agents with sun protection, such as imidazoles and zinc pyrithione shampoos, are common treatments. Oral regimens, including itraconazole, fluconazole, and pramiconazole, are also effective. Within a year, 60-68 percent of patients relapse, but once controlled, weekly anti-fungal shampoo or 200mg itraconazole twice a day, once monthly can prevent recurrence.
Paucibacillary leprosy: Caused by Mycobacterium Leprae, this disease progresses slowly, often appearing months or years after incubation following the onset of numbness or hyperalgesia. Indeterminate leprosy presents smooth, irregularly-bordered hypopigmented macules on the extremities and face. It can resolve, persist or progress based on the patient’s immune system. Tuberculoid and borderline leprosy often present with homogeneous hypopigmentation, erythema, and induration. Waning redness or repigmentation indicate resolution.
Macular post-kala-azar dermal leishmaniasis:
Leucoderma syphiliticum: Although the painless ulcer associated with primary syphilis can go undetected, secondary syphilis (which appears 6-8 weeks after initial infection) can cause hypopigmented macular eruptions with or without alopecia. It is usually preceded by erythema.
DISCRETE HYPOPIGMENTED MACULES
These conditions require little-to-no treatment.
Idiopathic Guttate Hypomelanosis (IGH): This chronic condition, associated with ultraviolet exposure, trauma and genetic factors, appears more with age and presents otherwise asymptomatic hypopigmented-to-depigmented macules over the extremities. If treatment is desired, approach cryotherapy carefully in patients with dark-colored skin - it can create dyspigmentation around macules.
Chronic arsenic exposure (CAE): Often mistaken for IGH, CAE produces hypopigmented or depigmented macules on the trunk and extremities. It occurs mainly in patients who use non-public water sources, herbal medicines or who live in farming communities using arsenic as a pesticide. Early recognition is vital due to life-threatening, long-term complications, including heart attack, liver damage, cognitive impairment, pulmonary disease, cancer, adverse pregnancy outcomes and peripheral vascular disease.
LYMPHOMA-ASSOCIATED HYPOPIGMENTATION
Hypopigmented parapsoriasis en plaque (PSEP): PSEP appears as smooth, oval or round hypopigmented macules or patches. Management is similar to HMF, and if treated with narrow-band UVB phototherapy, it can resolve within two years. Roughly 14 percent of cases progress to HMF.
Overall, investigators said, systematically assessing clinical presentations, gathering a thorough history, and conducting a physical examination, can increase the likelihood of pinpointing the proper diagnosis.
Reference:
Oussedik E, Picardo M, Saleem M, Schoch J, “Acquired disorders with hypopigmentation: A clinical approach to diagnosis and treatment,” Journal of the American Academy of Dermatology (2018); dio: 10.1016/jaad.2018.07.070.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.