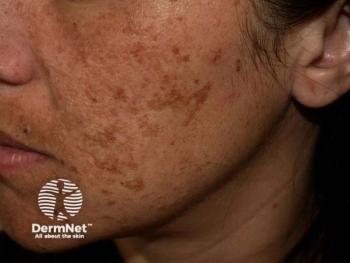
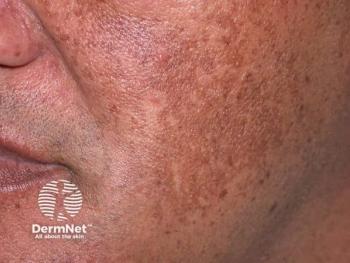
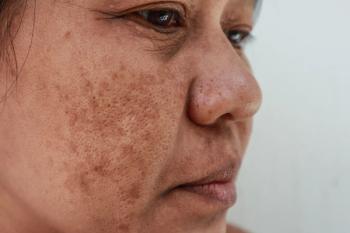
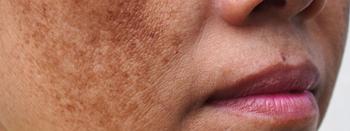
Dermoscopy serves dual role in melasma management
In patients with melasma, an in vivo imaging technique can effectively diagnose the condition as well as measure response to laser treatment, a recent study indicates.
Dermoscopy not only effectively diagnoses melasma but also ascertains the efficacy of low-fluence 1064 nm Q-switched Nd:YAG laser therapy used to treat it,
The fact that it can do both provides dermoscopy a clinical edge over using the modified melasma area and severity index (mMASI) and colorimetry, according to the paper.
“mMASI, colorimetry and dermoscopy had ascertained the efficacy of low-fluence 1064 [Q-switched] Nd:YAG laser in melasma; however, dermoscopy is superior to other assessments as it can help in the diagnosis of melasma besides the follow-up assessment and can precisely detect the detailed changes in response to treatment,” the authors write.
Studies have shown that dermoscopy can determine melasma’s depth, differentiate melasma from other facial pigmentation causes, monitor treatment outcomes and detect early treatment-related complications.
RELATED:
Today’s go-to melasma treatments range from regimens combining photoprotection, trigger avoidance and topically applied agents to laser and light source therapies. Laser toning with the low-fluence 1064 nm Q-switched Nd:YAG has been shown to effectively and safely treat melasma, although some studies suggest laser treatment might result in hypo-melanosis or rebound hyperpigmentation.
Korean authors of a paper
For this new study, dermatology researchers in Cairo, Egypt, analyzed dermoscopy’s roles in assessing melasma and monitoring treatment response post-Nd:YAG.
They studied 31 mostly female patients, who were 25 to 54 years old. The patients had a range of facial melasma distribution patterns and had melasma for 12 months to as long as 210 months. Patients hadn’t treated their melasma for at least three months prior to the study.
Researchers examined patients for the type and distribution of melasma. They treated patients with the 1064 nm Q-switched Nd:YAG laser at a fluence of 2 J/cm2, 8 mm spot size and 3 Hz frequency. They did three to four passes with the laser until the development of erythema but not petechiae.
Each patient had five laser sessions on affected areas at two-week intervals.
Researchers evaluated patients at baseline and two weeks after the final laser session, or at the 10th week. They compared mMASI sore, a subjective melasma assessment method looking at melasma involvement area and darkness; dermoscopic score of pigmentary and vascular melasma elements; and colorimetric evaluation placing the colorimeter perpendicular to the skin with minimum pressure.
They reported:
- mMASI scores improved significantly post-laser treatment, from 2.40 to 13.60 at baseline to 0.60 to 10.30 after treatment.
- Dermoscopic scores of pigmentary and vascular elements in melasma improved significantly from three to 11 at baseline to two to eight post-1064 nm Q-switched Nd:YAG treatment.
- Patients’ globular and perifollicular patterns improved significantly post-treatment.
- Colorimetric evaluation yielded melanin indices from 565 to 761 and erythema indices from 428 to 471 before treatment compared to melanin indices from 558 to 675 and erythema indices of 415 to 459 after laser treatment.
- There were no correlations noted among the three scores.
- Transient mild erythema was the only treatment-related side effect reported.
- Patient satisfaction scores revealed excellent improvement in seven patients; good improvement in 11; moderate improvement in 10; and poor improvement in 3 patients.
“The present study revealed significant improvement of melasma after [Q-switched] Nd:YAG laser that was proved by mMASI score as well as colorimetric melanin and erythema indices,” the authors wrote. “This significant outcome was confirmed by our simple practical ‘dermoscopic score of pigmentary and vascular elements.’ The dermoscopic globular and perifollicular pigmentary patterns had showed significant improvement, a finding that might help in deciding the prognosis of melasma.”
The authors say they think they didn’t see significant side effects from treatment because they used three to four passes compared to the five to 10 passes used by many other researchers. But they admit their study is limited by its small sample size, small number of laser sessions and lack of follow up.
Reference:
Abdel Hay, R, Mohammed, FN, Sayed, KS, Abd El Fattah, NA, Ibrahim, S. Dermoscopy as a useful tool for evaluating melasma and assessing the response to 1064‐nm Q‐switched Nd:YAG laser. Dermatologic Therapy. 2020;e13629.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.