CTCL varied in signs, symptons
San Francisco - In general, cutaneous T-cell lymphoma (CTCL) - a low-grade lymphoma that typically presents in or on the skin - can be hard to diagnose, according to Jacqueline M. Junkins-Hopkins, M.D., assistant professor, University of Pennsylvania Health System's department of dermatology, Philadelphia.
"The clinical and histological features of CTCL overlap with inflammatory diseases, like eczema and contact dermatitis. In addition, when CTCL is in its early phase, the features may be too subtle to make a diagnosis with certainty or it might be missed if the clinician is unaware of the diagnosis, and does not alert the dermatopathologist of the possibility of cutaneous lymphoma," she explains.
Cutaneous T-cell lymphomas are a heterogenous group of lymphoproliferative disorders caused by clonally-derived, skin-invasive T-cells. Mycosis fungoides (MF) and Sezary syndrome (an advanced form of MF) are the most common types of CTCL.
"In some cases, there are lesions that look like (CTCL) histologically and clinically, but they are due to a drug," Dr. Junkins-Hopkins explains.
Recently, the World Health Organization (WHO) and The European Organization For Research and Treatment of Cancer (EORTC) drafted a combined WHO/EORTC classification. Willemze, R et al., outline the new classification, which is now called the WHO-EORTC classification (Blood. May 15, 2005; 105(10):3768-3785). In this paper, the authors describe the characteristic features of the different primary cutaneous lymphomas and other hematologic neoplasms frequently presenting in the skin, and discuss differences with the previous classification schemes.
"This now promotes these skin restrictive diseases and shows how it is different from lymph node disease," Dr. Junkins-Hopkins tells Dermatology Times.
T-cell lymphoma variants
Dr. Junkins-Hopkins notes that CTCL presents itself as two main types: classic mycosis fungoides, including Sezary syndrome. Classic MF is the most common type of T-cell lymphoma, non-mycosis fungoides or non-epidermotropic CTCL.
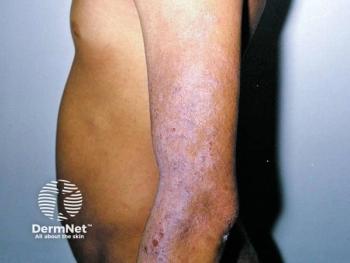
"The classic presentation progresses from scaly patches to plaque to tumors, but not all patients will progress in this fashion. There are some clinical variants where patients may have purpuric or hypopigmented patches, or the MF might be limited to their hands and feet," Dr. Junkins-Hopkins says.
Subtypes
There are several formal WHO/EORTC subtypes that have specific pathologic findings and a distinct clinical presentation.
Folliculotropic MF, with or without mucinosis. The lymphocytes mainly focus around the hair follicles. Patients have hair loss and acne type bumps.
Granulomatous slack skin, another MF subtype. Patients present with plaques in their armpits and their groins. With time, these plaques thicken and the elastic tissue is eroded away, according to Dr. Junkins-Hopkins.
"This is very rare and it may be associated with systemic lymphoma," she says.
Pagetoid reticulosis. Patients present with scaly plaques on the arms and legs. "Under the microscope there is a specific pattern where these lymphocytes are prominently in the epidermis (epidermotropic)," Dr. Junkins-Hopkins says.
There also are some other types of rarer and more aggressive subtypes of CTCL. Dr. Junkins-Hopkins also identifies variants of erythrodermic T-cell lymphoma, including Sezary syndrome, and erythrodermic MF. In Sezary syndrome patients present with diffuse redness of skin, with lymph node and blood involvement.
T-cell dyscrasias are conditions that may have a clone or may be associated with CTCL, but are not malignant at the outset, and include:
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.