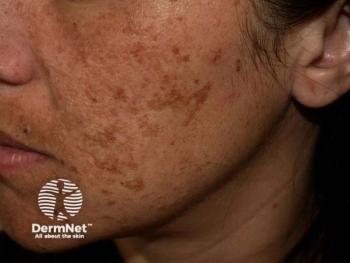
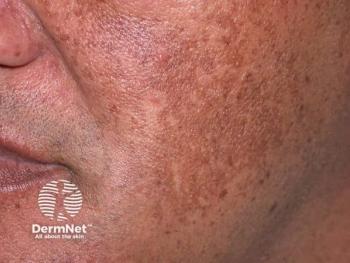
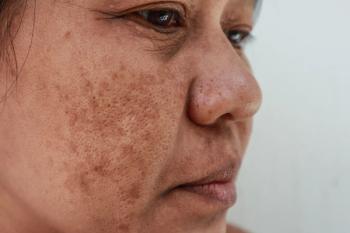
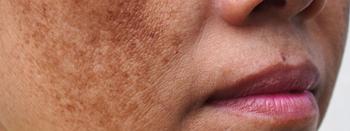
A closer look at tranexamic acid for melasma
A growing body of evidence supports treating melasma with systemic or intradermal tranexamic acid. But melasma patients often relapse when they stop taking the antifibrinolytic agent, and research on tranexamic acid’s long-term efficacy and safety is limited.
A growing body of evidence supports treating melasma with systemic or intradermal tranexamic acid. But melasma patients often relapse when they stop taking the antifibrinolytic agent, and research on tranexamic acid’s long-term efficacy and safety is limited, according to a recent
Discovered serendipitously as a urticaria and angioedema treatment, tranexamic acid’s popularity as a treatment for a wide variety of dermatologic conditions appears to be growing. Studies looking at using tranexamic acid for not only melasma but also post-inflammatory hyperpigmentation, urticaria, angioedema and hemostasis offer both encouraging and discouraging results.
And while the FDA has approved oral tranexamic acid for menorrhagia it has not yet approved it for treating skin conditions, including melasma.
Tranexamic Acid for Melasma
The most promising evidence supporting tranexamic acid as dermatologic monotherapy is in melasma treatment. Scientists believe tranexamic acid’s antiangiogenic and anti-melanogenic properties contribute to its efficacy in reducing melasma symptoms, according to the paper.
Researchers have studied treating patients with various doses and forms of tranexamic acid. They’ve found that the optimal dose depends on the condition being treated. In the cases of melasma and post-inflammatory hyperpigmentation, doses range from 4 mg/mL to 50 mg/mL, whereas the optimal dose for hemorrhage prevention is 100 mg/mL.
Most researchers have reported on oral or intradermal tranexamic acid administration. Fewer studies have focused on using topical tranexamic acid for melasma, according to the paper.
In what the authors say is the largest retrospective study of melasma and oral tranexamic acid treatment,2 researchers studied 561 melasma patients treated with 250 mg tranexamic acid taken twice daily, for an average of four months. Nearly 90% of patients improved within two months of treatment. The relapse rate among those who improved was 27.2%.
Adverse events occurred in 7.1% of patients studied, including one case of deep vein thrombosis, according to the
In a
The treatment methods were equally effective, reducing Melasma Area and Severity Index scores by about 78 in the oral group and 79 in the intradermal group at 12 weeks. Two patients had relapses at 24 weeks in the oral group but none relapsed in the intradermal group. Adverse events were mild.
In a study of 60 female melasma patients treated with topical tranexamic acid or topical hydroquinone, researchers found Melasma Area and Severity Index scores decreased significantly and comparably in both groups. But the hydroquinone group had more side effects and lower patient satisfaction compared to the tranexamic acid group, according to the
Some researchers have also reported synergistic effects from tranexamic acid combined with lasers and other topicals, according to the paper.
Side effects from tranexamic acid treatment for melasma tend to be mild but are numerous. Abdominal pain, bloating, nausea and vomiting, numbness or facial pruritus, tinnitus, transient amnesia, tremor, dysmenorrhea, hair shedding, facial hypertrichosis, lip or periorbital swelling and palpitations are among the most common adverse events from the medication, according to the paper.
Dermatologists and others should first educate patients about the rare risk of thromboembolic events. Among the contraindications for prescribing tranexamic acid: active thromboembolic disease; intrinsic risk of thrombosis or thromboembolism; pregnancy; severe renal insufficiency; if patients are taking Factor 9 complex concentrates or anti-inhibitor coagulant concentrates; and history of convulsions. Breastfeeding is among the relative contraindications.
Other Skin Conditions
Researchers studying tranexamic acid as prophylaxis against post-inflammatory hyperpigmentation report relatively little or no efficacy. As monotherapy, tranexamic acid has not been shown to successfully treat other facial dyschromia types, according to the authors.
Tranexamic acid does appear to reduce the frequency and severity of hereditary angioedema attacks for the long-term, according to the review paper.
The authors only cite a small study from 1979 suggesting oral tranexamic acid may reduce the frequency and severity of chronic urticaria.
Researchers have found tranexamic acid helps reduce perioperative bleeding. The authors of the review cite a couple of studies, one on Mohs micrographic surgery patients and another of patients undergoing dermatologic surgery, suggesting tranexamic acid reduced bleeding.
Case reports suggest tranexamic acid might help treat rosacea and wrinkles, the authors write.
References:
- Forbat E, Ali F, Al-niaimi F. The emerging importance of tranexamic acid in dermatology. Clin Exp Dermatol. 2019. Epub ahead of print.
- Lee HC, Thng TG, Goh CL. Oral tranexamic acid (TA) in the treatment of melasma: A retrospective analysis. J Am Acad Dermatol. 2016;75(2):385-92.
- Atefi N, Dalvand B, Ghassemi M, Mehran G, Heydarian A. Therapeutic Effects of Topical Tranexamic Acid in Comparison with Hydroquinone in Treatment of Women with Melasma. Dermatol Ther (Heidelb). 2017;7(3):417-424.
- Sharma R, Mahajan VK, Mehta KS, Chauhan PS, Rawat R, Shiny TN. Therapeutic efficacy and safety of oral tranexamic acid and that of tranexamic acid local infiltration with microinjections in patients with melasma: a comparative study. Clin Exp Dermatol. 2017;42(7):728-734.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.