Childhood cutaneous T-cell lymphomas on rise, experts say
National report - The two forms of cutaneous T-cell lymphomas (CTCL), mycosis fungoides (MF) and S?zary syndrome, are reported to arise more often in adults than in children. But the incidence of cutaneous T-cell lymphomas appears to be on the rise in children and adolescents.
This sobering fact has led clinicians to address and more closely analyze the morphologic variants, diagnosis, prognosis and management of CTCL in children and adolescents, according to Marie-France Demierre, M.D., F.R.C.P.C., associate professor of dermatology and medicine and director of the Skin Oncology Program at Boston University School of Medicine.
CTCL background
Dr. Demierre says that epidemiological data in the United States shows that CTCL occurs in 0.3/100,000 of the population, with children accounting for 0.5 to 5 percent of all CTCL cases reported. In classical MF, the disease is usually preceded by dermatitis for years and, more often than not, follows an indolent course.
"Cutaneous T-cell lymphoma can either be localized or generalized," Dr. Demierre says. "The youngest onset of symptoms has been seen at six months with the diagnosis made at 22 months, males being affected twice as (often) as females and T1 being more common than T4. In adults, the prognosis of CTCL by skin stage T1, T2, T3 and T4 at diagnosis is 100 percent 10-year relative survival; 67 percent; 39 percent; and 41 percent, respectively."
Children present more often in early stage and have a better prognosis than adults.
Mycosis fungoides in children
Dr. Demierre cites data from UCSF where MF with an onset in patients less than 20 years of age presented as a patch or plaque and represented 4.3 percent of all CTCL cases reported. None of the cases progressed to a more advanced stage (for up to 24 years, median for up to 12 years) and a stunning 21 percent had hypopigmented MF. The outcome of MF in the 34 patients with a male/female ratio of 2:1 in patients less than 16 years of age showed 50 percent with stage IA, 47 percent with stage IB and only 3 percent with IIA. These patients broke down into 24 percent with hypopigmented lesions, 26 percent with poikiloderma, 9 percent pilotropic and 18 percent lymphomatoid papulosis.
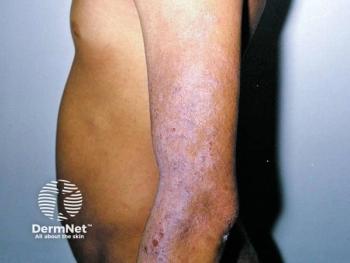
Dr. Demierre tells Dermatology Times, "Hypopigmented MF in children has an early onset and often occurs in dark-skinned children, but (it) can also be seen in Caucasians. Hypopigmentation can be the sole manifestation, or (it) can present as erythematous patches and plaques. These patients show a good response to therapy, phototherapy being a preferred choice, but, unfortunately, recurrences are common. The differential diagnoses in children include pityriasis alba/atopic dermatitis, vitiligo, post-inflammatory hypopigmentation and pityriasis lichenoides."
Folliculotropic MF has a follicular involvement with follicular mucinosis seen in the histology. Fortunately, there is a benign prognosis in children. Dr. Demierre says that this type of MF is only diagnosed in children if the evolution of the disease demonstrates progressive and persistent lesions. Topical treatment modalities include super-potent steroids, nitrogen mustard, topical bexarotene, off-label imiquimod and calcineurin inhibitors. Phototherapy as a monotherapy or in combination with retinoids has also proven to be successful. For large infiltrated lesions, Dr. Demierre advocates interferon-alpha subcutaneously with PUVA.
The third subtype of MF is granulomatous slack skin MF - very rare, and usually having an indolent course. Here, the folds are involved and there is an association with visceral lymphoma. Dr. Demierre believes that granulomatous slack skin in children is possibly a guarded diagnosis.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.