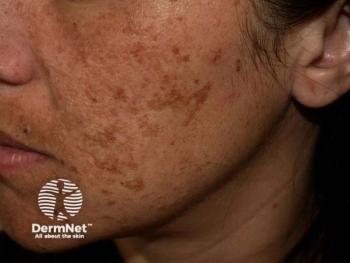
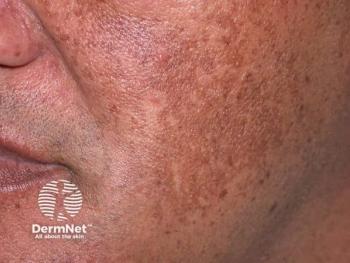
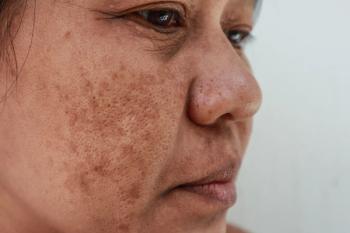
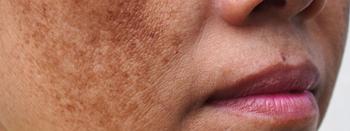
Characteristics that distinguish facial hyperpigmentation disorders
Effective treatment first requires accurate diagnosis, one expert says. He offers tips to distinguish melasma from other disorders and suggests some patients may need to be checked for diabetes and metabolic syndrome if they exhibit certain presentations.
By recognizing nuances in facial pigmentation, dermatologists can better diagnose and treat patients with facial hyperpigmentation, according to Amit G. Pandya, M.D., staff dermatologist at the Palo Alto Medical Foundation in Sunnyvale, Calif., and clinical professor of dermatology at University of Texas Southwestern Medical Center, Dallas.
Facial hyperpigmentation is common. And dermatologists will likely encounter patients with many of the more common facial pigmentation disorders, including lentigines, melasma, periorbital dark circles, drug-induced hyperpigmentation, acanthosis nigricans, lichen planus pigmentosus and maturational hyperpigmentation.
“… the first thing we have to do as dermatologists is determine the cause of this problem,” says Dr. Pandya, who presented “Unmasking Facial Hyperpigmentation,” during the American Academy of Dermatology VMX 2020.1
Distribution, presentation
Pigmentary distribution often helps dermatologists distinguish melasma, one of the most common of the disorders, from others.
Dr. Pandya pointed to these clues:
Melasma tends to involve the central area of the forehead; whereas, lichen planus pigmentosus is more likely the diagnosis when lateral areas of the forehead are involved.
“Melasma often occurs in the area above the eyebrow or under the eyebrow. However, it does not cross the superior orbital rim and does not go above the inferior orbital rim. That presentation is simply called dark circles around the eyes,” he said during the presentation. “Melasma does commonly go over the bridge of the nose, but it does not affect the tip of the nose. If it’s on the tip of the nose, that’s often seen with sarcoidosis and drug-induced hyperpigmentation.”
Whereas patients with melasma might have pigmentary changes on the zygomatic prominence, patients with acanthosis nigricans more likely have hyperpigmentation on the concave area below the zygomatic prominence.
Melasma tends to occur above the mandible, versus poikiloderma of Civatte, which occurs below the mandible.
And while the nasolabial fold usually is spared in melasma, it isn’t in seborrheic dermatitis or drug-induced hyperpigmentation.
Lentigines, often presenting as asymmetrical, well-circumscribed hyperpigmented macules, are more common in Asians, according to Dr. Pandya.
“… they tend to be not as symmetrical as melasma and scattered in various sun-exposed areas of the face areas,” he said.
Hyperpigmentation that’s somewhat bluish and which can extend, below the jawline, could be drug-induced hyperpigmentation, as in a case of minocycline pigmentation that Dr. Pandya illustrated. Another patient with hyperpigmentation below the jawline, on the tip of the nose, the nasolabial folds and the eyelids, which are not typical locations for melasma, had drug-induced hyperpigmentation from a nonsteroidal anti-inflammatory drug.
A patient presenting with hyperpigmentation strictly around the eyes and not on the cheeks may have dark circles around the eyes, which is usually due to increased epidermal and dermal melanin, he says.
Dr. Pandya presented a case in which the patient had hyperpigmentation of the temples, as well as a straight line going over his zygomatic prominence. The straight line is known as pigmentary demarcation line F, whereas the pigmentation of the temples is due to acanthosis nigricans. Some call it maturational hyperpigmentation, according to Dr. Pandya.
Dermatologists should consider checking some of these patients for diabetes and metabolic syndrome, he says. He referred to a study of 123 patients with acanthosis nigricans compared to sex- and age-matched controls.2
“The mean age of onset was 31 years. There was elevated insulin in 37%. It was associated with male gender, positive glucose tolerance test, increased waist-hip ratio and increased body mass index,” he says. “When you see patients with this greyish hyperpigmentation going up the temple and in the area under the zygoma, it may be worthwhile asking about risk factors for diabetes and metabolic syndrome, perhaps even checking some laboratory tests. We still don’t have very data to see if this all goes away with weight loss and control of these disorders.”
Pigmentary demarcation lines that coalesce with dark circles around the eyes is common in the South Asian population, according to Dr. Pandya.
“You have to be able to distinguish between [demarcation lines] and melasma and other disorders. Unfortunately, pigmentary demarcation lines are genetically determined so these patients tend to have them throughout their lifetime. They are difficult to treat and they get worse during the summer,” he said.
Examining patients is an important part of diagnosing facial pigmentary disorders. History-taking and, sometimes, other testing helps to determine the exact diagnosis, he said.
“Effective treatment first requires a correct diagnosis,” according to Dr. Pandya.
Disclosures:
Dr. Pandya is a consultant for Incyte, Pfizer, Viela Bio, Villaris; and investigator for Incyte, Pfizer and Immune Tolerance Network; and has stock options with Clarify Medical and Tara Medical Devices.
References:
1 Pandya, A. Unmasking facial hyperpigmentation. Presented at American Academy of Dermatology Virtual Meeting Experience 2020, June 12-14, 2020.
2 Panda S, Das A, Lahiri K, et al.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.