An Overview of Harlequin Ichthyosis
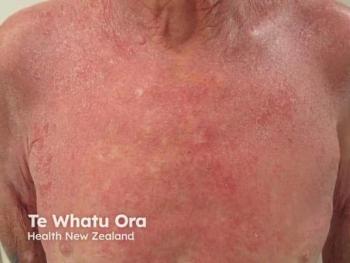
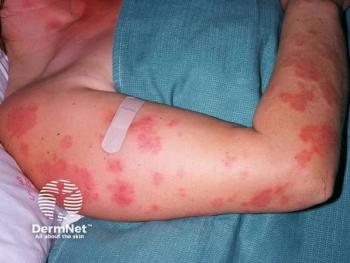
Harlequin ichthyosis is a rare skin disorder with thick, large, plate-like scales over the entire body that later develop into erythroderma.
Harlequin ichthyosis (HI), the most severe form of ichthyoses, is a rare genetic disorder affecting 1 in every 3,000,000 neonates.1 The disease is characterized by stiffened and splitting skin and is associated with a high mortality rate due to the possibility of skin infections, respiratory distress or loss of fluid.1
Clinical Presentation:
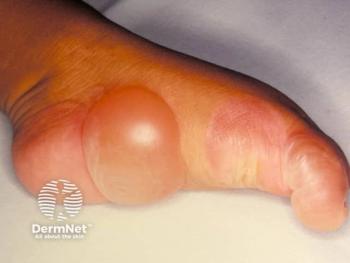
HI, often called ichthyosis fetalis, is a rare skin disorder with thick, large, plate-like scales over the entire body that later develop into erythroderma.2 The condition causes extreme hyperkeratosis in the stratum corneum.3 Neonates with HI are born with extremely thickened skin that leads to impaired skin barrier function, prone to skin infections and loss of fluid, requiring intensive interprofessional care.4 Data show that fulminant sepsis and respiratory failure are the most common causes of death among patients with HI.3
Severe eclabium, ectropion, flattened and poorly developed ears and nose, and limited mobility of joints are some of the clinical features associated with the disease.5 Studies have reported recurrent skin infections in early childhood and delayed walking due to palmoplantar keratoderma.3 Nail deformities, poor hair growth, difficulty in weight maintenance despite being on a high-caloric diet, and ophthalmic conditions, including keratitis, conjunctivitis, and ectropion, have also been reported among patients with HI.3
Causes:
HI is mainly caused by mutations in the ABCA12 gene, a lipid transporter essential for the development and maintenance of the epidermal lipid barrier. Neonates with this mutation have abnormal lipid transportation to epidermal keratinocytes, affecting the normal skin lipid barrier.2 Excess of lipids inside the epidermal keratinocytes gives rise to the morphological features commonly seen with HI.3
Diagnosis:
Prenatal diagnosis is crucial for perinatal and postnatal management of the condition and may help prepare parents for successive pregnancies. In patients with a family history, prenatal testing via DNA analysis of the fetus may be offered. Sonography is a key method in detecting HI. Discontinuity in ultrasound is an indicative feature of thickened skin. Moreover, this two-dimensional method also detects macroglossia, flexion contracture, digital shortening, convex lips, and open mouth, all of which are critical features of HI. However, the method is unable to differentiate HI from other fetal conditions exhibiting characteristics like macroglossia, including Down syndrome and congenital tumors like infantile hemangiomas. Therefore genetic testing is crucial to differentiate HI from other fetal genetic disorders.2 After discovering mutations in the ABCA12 gene, the diagnosis is confirmed by amniotic fluid or chorionic villi sampling.1
Moreover, the three-dimensional ultrasound can aid in the diagnostic process of the two-dimensional method by visually displaying abnormalities in the fetus and explaining to parents the exact nature of the disease. However, it cannot replace the two-dimensional method since most cases develop in the third trimester when there is less amniotic fluid.1
Treatment:
Admitting neonates with HI to NICU under the care of a multidisciplinary team is required for early intervention. Immediate actions are needed to prevent electrolyte imbalances, malnutrition, respiratory failure and infections. All these measures increase the survival rate and can optimally be performed in the NICU.6
To ease discomfort associated with scaly skin, most neonates require narcotic pharmaceuticals. Newborns with eclabium and limited mouth opening that may interfere with feeding require nasogastric or oropharyngeal tube feeding.6 Studies have also reported vitamin D deficiency as a crucial risk factor for causing severe skin scaling in patients with HI.7 Thus, continuous monitoring of vitamin D levels and supplementations are needed to manage HI infants.6 Topical ointments and surgical interventions, including full-thickness autografts from engineered human skin or the auricular skin, have been proven effective in correcting ophthalmic issues.8
Retinoids are another class of drugs that have revolutionized the lives of many patients with HI. Topical retinoids, such as tazarotene cream at a 0.1% concentration, and the soft splinting of feet and hands are effective alternative therapeutical interventions to avoid surgery.6 Moreover, acitretin helps in reducing scales, thus thinning hyperkeratosis. It also helps improve hypohidrosis, hearing ability, and hair growth and helps manage ectropion and eclabium.9 However, a randomized, double-blinded study suggested using vitamin D as an alternative to acitretin in treating congenital ichthyosis to avoid associated side effects.10
A study highlighted the importance of oral retinoids in improving survivability among patients with HI and reported that 83% of the patients treated with oral retinoids survived, whereas 76% of patients who didn't receive the treatment died.3
Although retinoids have been proven effective in softening hyperkeratinic bands, critical limb ischemia requires immediate surgical management.7 However, surgical procedures come with their own risks, such as the possibility of infection on the wound site and iatrogenic injury, which may complicate the condition.
Overall, the management of HI, both surgically and systematically, can be quite tricky. Healthcare professionals should be highly cautious while opting for invasive procedures due to the high possibility of sepsis and infections.
References
- Zhou Y, Li L, Wang L, Zhang C. Prenatal diagnosis of a rare variant of Harlequin Ichthyosis with literature review. BMC Medical Imaging. 2021;21(1). doi:10.1186/s12880-021-00586-4
- Liang Q, Xiong F, Liang X, et al. Two successive cases of fetal Harlequin Ichthyosis: A case report. Experimental and Therapeutic Medicine. 2018. doi:10.3892/etm.2018.6917
- Elkhatib AM, Omar M. Ichthyosis Fetalis. [Updated 2022 Aug 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing;2022 Jan
- Enjalbert F, Dewan P, Caley MP, et al. 3D model of Harlequin Ichthyosis reveals inflammatory therapeutic targets. Journal of Clinical Investigation. 2020;130(9):4798-4810. doi:10.1172/jci132987
- Shrestha A, biswas prince, shrestha sajina, et al. Harlequin Ichthyosis: A case report and literature review. 2022. doi:10.22541/au.166436940.09885846/v1
- Tsivilika M, Kavvadas D, Karachrysafi S, Sioga A, Papamitsou T. Management of Harlequin Ichthyosis: A brief review of the recent literature. Children (Basel). 2022;9(6):893. Published 2022 Jun 15. doi:10.3390/children9060893
- Margulies IG, Harburg L, Zellner E. Surgical management of Harlequin Ichthyosis. Plast Reconstr Surg Glob Open. 2019;7(5):e2161. Published 2019 May 21. doi:10.1097/GOX.0000000000002161
- Karadağ R, Sevimli N, Karadağ AS, Wollina U. Successful correction of ichthyosis-related ectropion by autografts. Dermatol Ther. 2020;33(6):e13851. doi:10.1111/dth.13851
- Mazereeuw‐Hautier J, Vahlquist A, Traupe H, et al. Management of Congenital Ichthyoses: European guidelines of care, part one. British Journal of Dermatology. 2018;180(2):272-281. doi:10.1111/bjd.17203
- Bakshi S, Mahajan R, Karim A, De D, Handa S, Saikia B. Oral vitamin D versus acitretin in congenital non-syndromic ichthyosis: double blinded, randomized controlled trial. J Dtsch Dermatol Ges. 2022;20(3):297-304. doi:10.1111/ddg.14666
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.