- General Dermatology
- Eczema
- Alopecia
- Aesthetics
- Vitiligo
- COVID-19
- Actinic Keratosis
- Precision Medicine and Biologics
- Rare Disease
- Wound Care
- Rosacea
- Psoriasis
- Psoriatic Arthritis
- Atopic Dermatitis
- Melasma
- NP and PA
- Skin Cancer
- Hidradenitis Suppurativa
- Drug Watch
- Pigmentary Disorders
- Acne
- Pediatric Dermatology
- Practice Management
AMA Streamlines Billing CPT Codes
This is the first overhaul in a quarter century that simplifies evaluation and management and increases flexibility.
A result of the first major overhaul in 25 years, the 2021 Current Procedural Terminology (CPT) code set published by the American Medical Association (AMA) incorporated foundational changes that ease evaluation and management (E/M).1
Wholesale changes to CPT E/M coding that took effect January 1, 2021, streamline billing documentation for dermatologists,” said Mark D. Kaufmann, MD, chief medical officer at Advanced Dermatology and Cosmetic Surgery in Maitland, Florida, in his presentation at Maui Derm Live. The in-person dermatology continuing medical education (CME) conference in Hawaii was held concurrently with Maui Derm Connect, a virtual CME conference, January 25 to January 29, 2021.
Table – CPT E/M Office Revisions Level of Medical Decision Making (Courtesy of the American Medical Association)
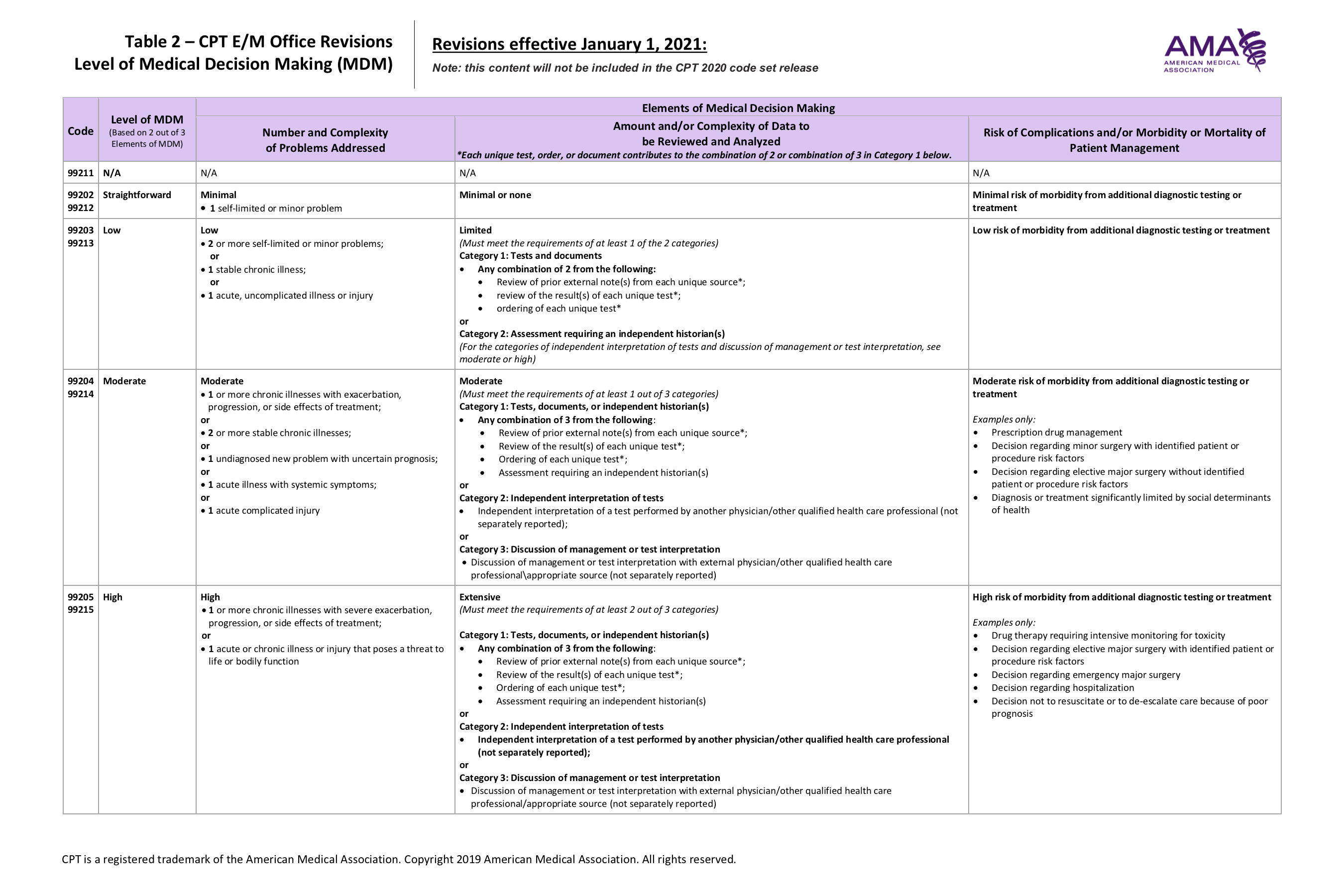
These changes would result in a shift in billing patterns for dermatologists, Kaufmann added. He likened the new 5-column grid1 used for coding E/M services to the Bible stating that, “This is the guidance that the AMA has given us—a 1-page graphic with language that is broadly open to interpretation.”2 Kaufmann is also clinical associate professor of the Department of Dermatology at the Icahn School of Medicine at Mount Sinai New York and an advisor to the American Academy of Dermatology Relative Value Scale Update Committee.
Dermatologists must use information from 2 of the 3 medical decision-making (MDM) columns in the code set to support the codes they bill, Kaufmann said. For example, androgenetic alopecia automatically merits a moderate (level 4) degree of MDM because it is a chronic condition that progresses. Dermatologists can choose level 4 in the first MDM column, Number and Complexity of Problems Addressed.
According to Kaufmann, a dermatologist prescribing a medication such as finasteride for androgenic alopecia can document this activity in the third MDM column, Risk of Complications and/or Morbidity or Mortality of Patient Management. With this example of moderate MDM in column 3, the dermatologist should have “moderate” in columns 1 and 3. Accordingly, the dermatologist could code the visit at 99204 or 99214, he says.
If the physician recommends an OTC medication such as minoxidil, this qualifies for low- level MDM, making the visit level 3 instead of 4. Counseling a patient without recommending treatment represents a straightforward MDM, a level 2 visit.
According to Kaufmann, medical dermatologists will “live” primarily at the low and moderate levels. Among the MDM columns, there will be appropriate occasions for column 2, such as when Mohs surgeons undertake patient consultations known as Amount and/or Complexity of Data to be Reviewed and Analyzed. “But in general dermatology, I have found that if you’re looking to get to a moderate level of MDM, a level 4 visit in column 2, you’re probably already there with columns 1 and 3,” he noted.
Risk levels associated with specific treatments require interpretation, Kaufmann said. For example, prescription drug management (an intervention option in the third column) corresponds with a moderate risk level. “Prescription drug management is a very broad statement,” he said. “In this regard, the AMA has said that even if a physician discusses a systemic drug with a patient and the patient refuses the drug, that’s prescription drug management. You don’t have to write the prescription. On the flip side, you have to decide where you sit when a patient says, ‘I need the same triamcinolone prescription you gave me last year for my winter’s itch.’”
Dermatologists must determine whether they are comfortable calling this interaction prescription drug management for billing purposes. “Everyone has to define the lines in their own minds," he said. "In my opinion, when patients come in for refills of systemic drugs, that’s always prescription drug management because you’re going to be talking about the drug with the patient.”
In Kaufmann’s view, financial implications of the E/M changes are likely to provoke payer anxiety. Initially, the Centers for Medicare & Medicaid Services (CMS) estimated that the changes’ net impact would be neutral or even feature a 1% cost reduction. The stimulus package signed by President Donald Trump in December 2020 turned the expected impact into a 5% cost increase.
The boost is helpful for 2021, according to Kaufmann. “But that doesn’t do anything for us in 2022 and beyond,” he said. “I’m sure that many of us will go to Capitol Hill later this year with the American Academy of Dermatology and other groups to ask that this fix be extended. But there’s no guarantee that it will be. And next year, we may be in the same position we were prior to the stimulus bill being signed.”
CMS’ cost estimates rested on the expectation that in 2021, the number of codes used at each level would remain the same as in 2020, but 99201 was eliminated. More importantly, Kaufmann expects 99202 usage to decline this year because many of these visits will shift to 99203. “I believe that many of the 99203s will shift to 99204, which was hardly perceptible up until January 2021,” he noted.
According to Kaufmann, CMS did not consider those dynamics when formulating their predictions. “We are probably going to see more audits,” he said, “which may lead to further deliberations on how to deal with these new realities.”
Disclosures:
Kaufmann is adviser to the American Association of Dermatology RVS Update Committee. He also owns stock in Modernizing Medicine and stock options in Klara.
References:
1. CPT evaluation and management (E/M) office or other outpatient (99202- 99215) and prolonged services (99354, 99355, 99356, 99XXX) code and guideline changes. September 1, 2020. Accessed January 26, 2021. https:// www.ama-assn.org/system/files/2019-06/cpt-office-prolonged-svs-code-changes.pdf
2. Kaufmann MD. How to maximize your billing effectiveness in the era of dwindling reimbursements and ICD-10. Presented at: Maui Derm For Dermatologists 2021; January 25-29, 2021; Maui, Hawaii.
