- General Dermatology
- Eczema
- Alopecia
- Aesthetics
- Vitiligo
- COVID-19
- Actinic Keratosis
- Precision Medicine and Biologics
- Rare Disease
- Wound Care
- Rosacea
- Psoriasis
- Psoriatic Arthritis
- Atopic Dermatitis
- Melasma
- NP and PA
- Anti-Aging
- Skin Cancer
- Hidradenitis Suppurativa
- Drug Watch
- Pigmentary Disorders
- Acne
- Pediatric Dermatology
- Practice Management
Arthritis in psoriasis not as common as we once thought
The prevalence of psoriatic arthritis in patients with psoriasis worldwide appears to be around 20 percent, shows a meta-analysis published in JAAD.
The prevalence of psoriatic arthritis in patients with psoriasis worldwide appears to be around 20 percent, shows a meta-analysis published in JAAD. (©TernavskaiaOlgaAlibec/Shutterstock.com)
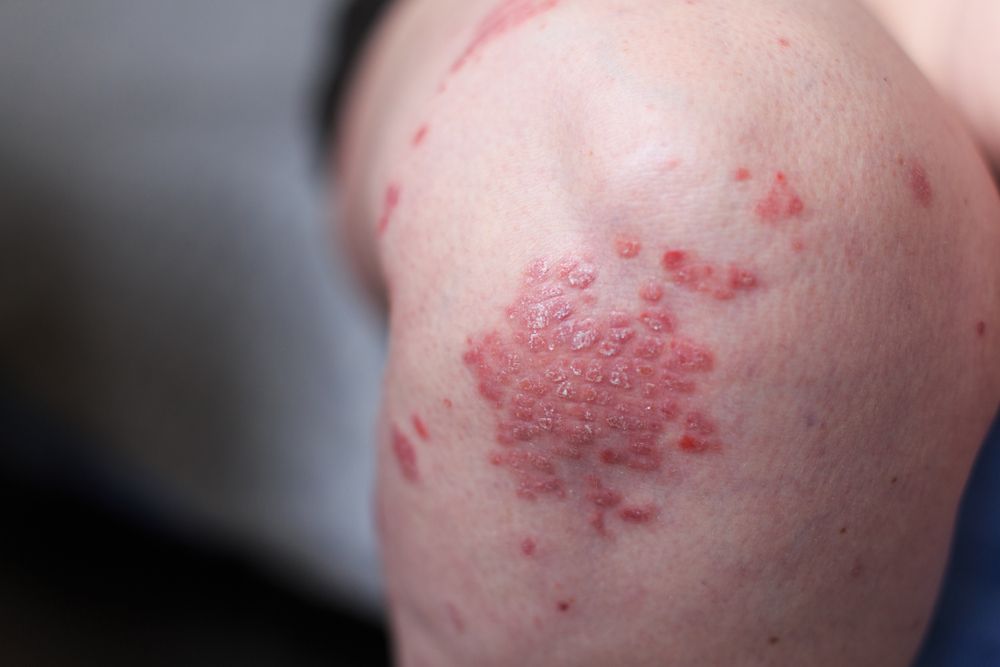
The prevalence of psoriatic arthritis (PsA) in patients with psoriasis worldwide appears to be around 20 percent, shows a meta-analysis published online June 18 in the Journal of the American Academy of Dermatology.
"When we give lectures, we all have slides that say the prevalence of psoriatic arthritis in patients with psoriasis is five percent to as high as 42 percent," said study co-author Jashin J. Wu, M.D., of Kaiser Permanente Los Angeles Medical Center, Los Angeles. "This meta-analysis narrows it down to 20 percent."
Dr. Wu and colleagues searched the PubMed, Web of Science and EMBASE databases from inception through November 2017, using the terms "psoriasis and psoriatic or arthritis o arthropathy or incidence or prevalence." Dr. Wu and colleagues identified 41 additional studies by screening references of studies found through their original search.
The analysis included patients with psoriasis and with PsA prevalence expressed as absolute figures or percentages. Researchers excluded studies that failed to specify the type of arthritis or used the catchall terms "psoriatic arthropathy," and "juvenile idiopathic arthritis (JIA)," as such studies may have included several types of arthritis.
The final analysis included 266 studies which included 976,408 patients with psoriasis, showing a pooled PsA prevalence of 19.7 percent (95% CI).
Worldwide prevalence estimates for adults remained fairly consistent when researchers divided data into various subpopulations. For example, 245 studies that reported PsA data in adults with psoriasis yielded a pooled prevalence of 21.6 percent. Likewise, 36 studies that stratified findings by gender showed PsA prevalence rates of 23.3 percent for men and 24.0 for women. Additionally, 45 studies that used the Classification for Psoriatic Arthritis (CASPAR) criteria found a pooled prevalence of 23.8 percent.
The congruence of estimates from Europe (22.7 percent, 119 studies) and North America (19.5 percent, 47 studies) agrees with findings from prior studies, the authors wrote. Regarding individual countries, investigators found PsA rates of 19.0 percent, 19.4 percent, 20.5 percent and 19.2 percent, respectively, for the United States (36 studies), the United Kingdom (10 studies), Germany (12 studies) and the Netherlands (11 studies).
Among 122 studies that included patients with moderate-to-severe psoriasis, investigators found a pooled prevalence of 24.6 percent, a figure which they said suggests that these patients require increased attention.
"It is generally accepted that PsA is uncommon in children, which is supported by the pooled prevalence of 3.3 percent," the authors added. This figure comes from 21 pooled studies of children and adolescents. Lack of clear segregation of PsA from JIA may partly explain the low estimate. However, said the authors, the fact that juvenile PsA represents approximately five percent of patients with JIA and that PsA often presents before psoriasis in children underscores the importance of distinguishing it as a separate entity from JIA.
Investigators observed decreasing proportion estimates as study population sizes increased.
"This might partly be explained by more thorough examination of psoriasis patients in smaller studies and underdiagnosis of PsA in larger ones; e.g. in register-based studies where PsA assessment is based on diagnostic codes, as such studies may tend to predominantly capture those patients with more severe joint symptoms," the authors wrote. Reported PsA incidence rates ranged from 0.27 per 100 person-years to 2.7 per 100 person-years.
Researchers found a high degree of heterogeneity in studies both overall and across virtually all subgroups. "Such heterogeneity may be attributed to the lack of widely accepted diagnostic criteria in the past, different study designs, geographical variations, ethnicity, the remitting and relapsing nature of the disease, and study inclusion criteria; e.g. whether patients with psoriasis were selected from primary, secondary or tertiary care settings."
Study limitations include its exclusion of studies written in languages other than English, and a significant risk of publication bias (Egger test p<0.0001) for all studies included.
Dr. Wu said that he and his co-authors hope their findings will make dermatologists more likely to screen patients with psoriasis for PsA, and that the study reminds physicians to prescribe biologic medicines approved for both psoriasis and PsA in patients with both conditions.
REFERENCE
Alinaghi F MD, Calov M MD, Kristensen LE MD, et al. "Prevalence of Psoriatic Arthritis in Patients with Psoriasis: a Systematic Review and Meta-Analysis of Observational and Clinical Studies," Journal of the American Academy of Dermatology. June 2018.
DISCLOSURES
Dr. Wu is an investigator for AbbVie, Amgen, Eli Lilly, Janssen, Novartis and Regeneron. No sources of funding were received for the preparation of the article discussed herein.
